 Faculty
Faculty
- Stephen A. Esper, MD, MBA, Medical Director
- Jennifer M. Holder-Murray, MD, FACS, FASCRS, Surgical Director
- Michael L. Boisen, MD, FASE
- Connie Chaudhary, MD
- Sean Dechancie, MD
- Brian Gierl, MD
- Murat Kaynar, MD
- Sharad Khetarpal, MD
- Joshua Knight, MD
- Stephen McHugh, MD
- Claudia Mulock, MD
- Kathirvel Subramaniam, MD, MPH, FASE
- Harikesh Subramanian, MD
- David Wang, MD
- Cynthia Wells, MD
Staff
In the current healthcare landscape, identifying and reducing mortal and morbid surgical risks is important for patients, families, providers, and healthcare systems. Patients identified as “high risk” based on their underlying physical status and co-existing medical conditions are associated with considerable morbidity and mortality and low-value care, accounting for more than 30% of ICU admissions, 70% of post-operative deaths, and 90% of the care provided during hospitalization. “Prehabilitation” of high-risk patients prior to surgery has been shown to help reduce hospital length of stay, hospital acquired conditions, and readmission rates, translating into better quality care, higher patient satisfaction, and cost savings.
The Center for Perioperative Care (CPC), a team-based, multidisciplinary prehabilitation clinic, identifies and screens high-risk patients prior to non-emergency surgery. The CPC accepts all patients under consideration for these surgical procedures and tailors the surgical experience to each patient's specific needs. This “surgical pause” provides the opportunity to mitigate risk and optimize patients’ health before surgery to improve outcomes or refer patients to safer non-surgical approaches if warranted. Anesthesiologists specializing in perioperative medicine facilitate the multidisciplinary CPC team, which includes the surgeon, primary care provider, and specialists working with the patient in a shared-decision-making approach. We have CPC clinics at five sites: UPMC Horizon, UPMC Jameson, UPMC Montefiore, UPMC Passavant, and UPMC Shadyside.
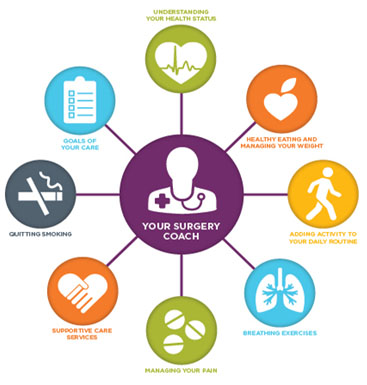
Patients seen in the CPC are assessed using a validated and accepted Risk Analysis Index tool developed by the CPC team to identify those at high-risk for poor surgical outcomes (see Arya S et al. Recalibration and External Validation of the Risk Analysis Index: A Surgical Frailty Assessment Tool. Ann Surg. 2019 Mar 19). The team’s comprehensive system addresses patients’ anesthetic and medical concerns, nutritional status, physical and cardiopulmonary therapy, weight loss, chronic pain assessment, and tobacco, drug, and alcohol cessation and provides mental health therapy and social work support services. At-risk patients are provided with a supportive “Surgery Coach” specifically trained in surgical preparation who mentors patients, readying them for their surgical experience.
For more information, please visit UPMC’s Center for Perioperative Care website.
